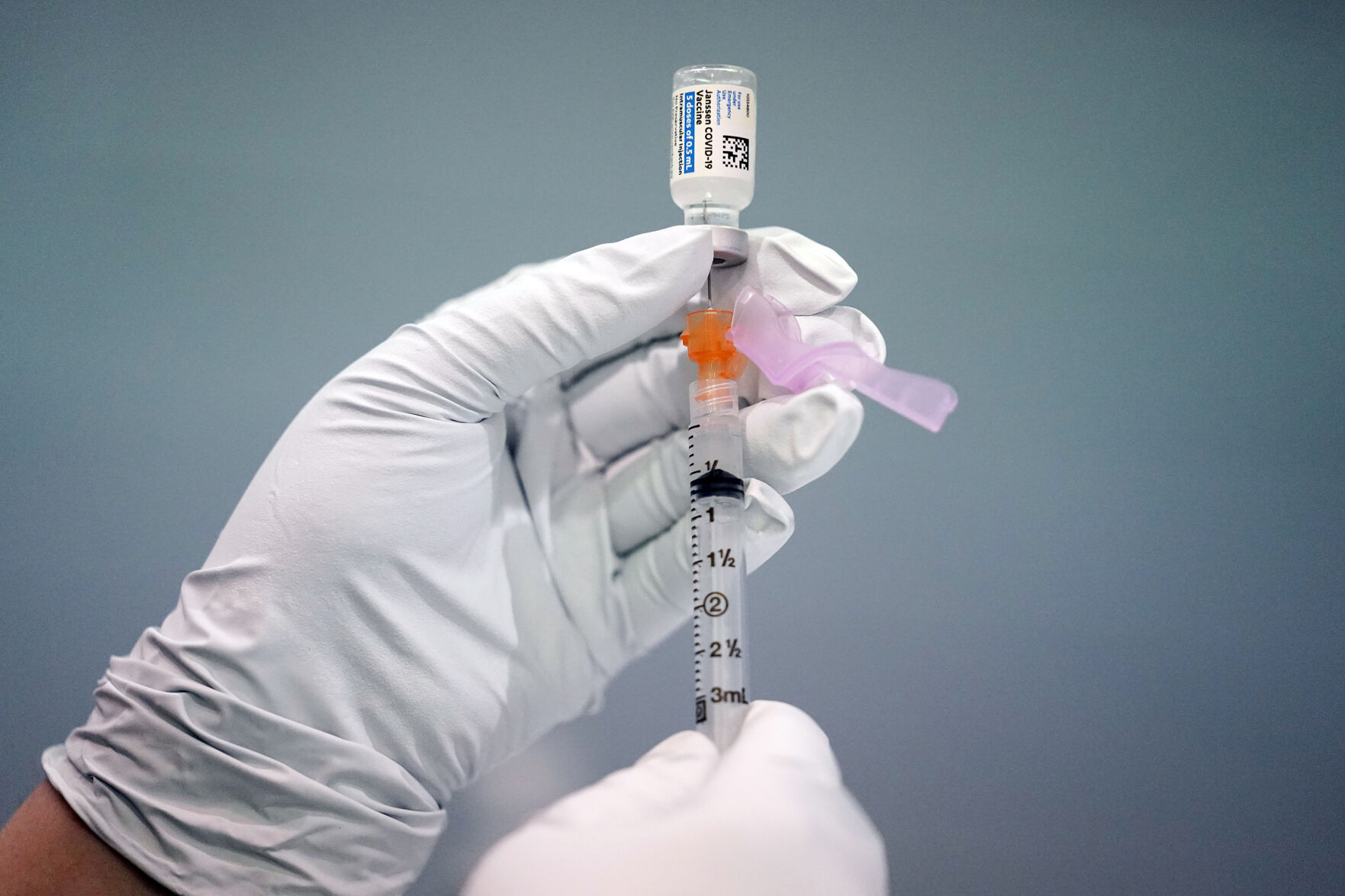
Colorado leads nation for high rate of COVID cases, but infections, hospitalizations here continue to drop
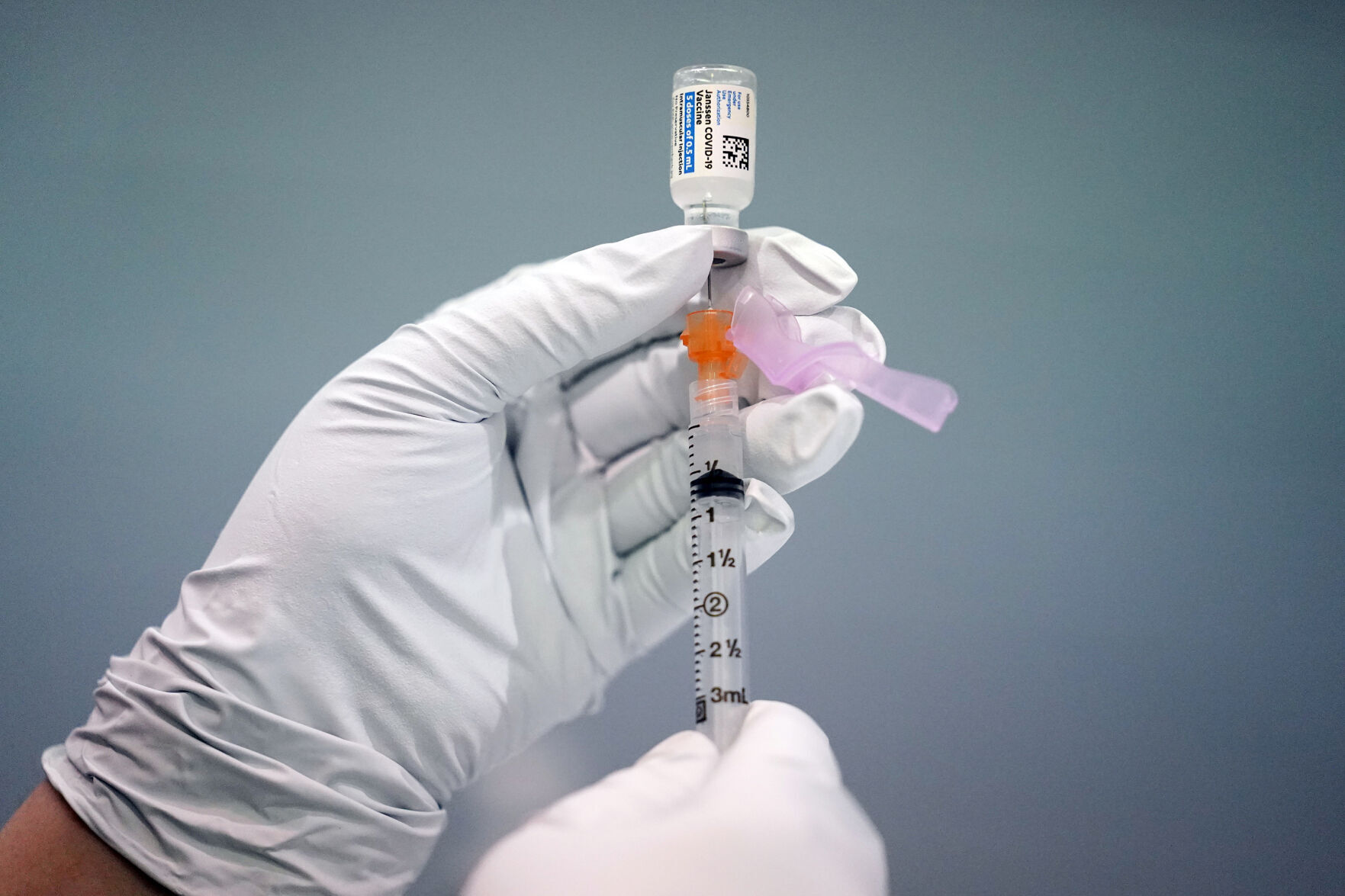
Colorado is leading the nation with the highest rate of new coronavirus cases over the past seven days, federal data shows. But the spread of the virus is slowing across the state and nationally, and though the numbers show Colorado is behind other states, COVID-19 metrics here are lower than at any point since March and far below fall spikes.
The Center for Disease Control and Prevention data show Colorado is seeing about 145 new COVID-19 cases per 100,000 people on average over seven days. Alabama has the second highest rate of cases, followed by Maine and Minnesota. The state is far outpacing all of its neighbors for new cases, none of which are in the top 10.
According to state data, Colorado is averaging about 968 cases each day over the past week. That’s the lowest total since March and a 44% drop from the most recent peak on April 25. Hospitalizations, which have become a key metric in gauging the severity of the pandemic, have fallen steadily for 10 days; confirmed COVID-19 hospitalizations are down 23%, and suspected cases are down 29%.
At the same time, Colorado boasts a relatively high vaccination rate, with 41% of the population, or about 2.38 million people, now fully vaccinated, the federal data show.
Experts cautioned against reading the CDC’s rankings the same as you would in the fall, when no vaccine was available and an increase in cases lead to a significant increase in hospitalizations and, later, deaths.
“Unfortunately I don’t have a great deal of clarity regarding why our case volume is so high compared to other states,” said Glen Mays, of the Colorado School of Public Health. “But the good news is that this case volume is not causing increases in severe illness and hospitalizations. So we can assume that most of this transmission is occurring among healthy and asymptomatic or mildly symptomatic people.”
He added that variants – primarily the more transmissible U.K. strain – are dominant here and could be driving higher growth than in other states.
Jen Tolbert, the director of state health reform for the national Kaiser Family Foundation, said that nationally, “we are in a good place in terms of cases and obviously deaths and hospitalizations.” But there remain “outbreaks and pockets of outbreaks” in some states and that “we haven’t beaten COVID.”
Because vaccines have blunted hospitalizations and deaths, rates of spread don’t provide the same gauge of “how bad it is or how bad the pandemic is nationally,” she said.
“But what the data are telling us where there may be some kind of unique set of factors that may be contributing to a sort of more isolated outbreak,” Tolbert said.
For Colorado, like Michigan, the data is likely saying that dominant variant strains played a significant part in the fourth pandemic wave that emerged during April and has largely begun to abate now. She cautioned against “overhyping” the CDC ranking and putting it into context: that the pandemic’s current status is a significant improvement from months ago.
Colorado is “definitely” seeing more cases than anytime since the fall surge, Tolbert said, but she said that cases are declining and the fourth peak has passed. Vaccination rates also indicate that cases should continue to decline. That, she said, is an important message, which Gov. Jared Polis and other top state officials have stressed: High vaccination rates translate to lower infection rates.
According to a modeling report released last week by researchers with the school of public health, cases appear to be flattening. Whether that continues, the researchers wrote, depends on infection control measures and how successful the state – and its residents – are at limiting the spread of the virus.
But many of those infection control measures, like masking and social distancing, have ended, at least as a required policy. If that leads to fewer people masking on their own or observing social distancing, along with projected increases in people leaving their homes and socializing, then “the epidemic curve (could remain) at current levels for several months to come,” according to the report.
Jon Samet, the dean of the school of public health and a member of the modeling team, said in an email that the epidemic curve “is now clearly descending.”
“However, the bad news is that the descent is beginning from a relatively high point after the curve went up over the last two months,” he said. “We have sought explanations for why Colorado has not done as well as other states. There is no immediately obvious explanation.”
Even with the declining numbers, the modelers project that with current trends, Colorado won’t hit its low summer 2020 levels until August. Indeed, the researchers estimated that even with high levels of vaccination uptake, the state won’t hit the minimum threshold to reach herd immunity – 70% of the population inoculated – until August at the earliest.
Both Samet and Mays noted that the state had “relatively good control” earlier in the pandemic, as Samet put it, which means that a “relatively large population (is) at risk as we began to relax control measures. In other words, because Colorado had done relatively well to control the pandemic previously, there are more people who aren’t immune and thus susceptible to illness.
Polis announced last week that he was largely lifting the statewide mask mandate, leaving many businesses and other private property owners to make their own decisions about mask requirements.
Colorado was one of several states to relax their mask orders after the CDC announced that vaccinated people can safely go without masks.
Some residents’ perception that it’s safe to go without masks even they are unvaccinated could be chalked up to communication “fumble” nationally that did not make it clear that the risks still exists for them, said Phoebe Lostroh, a Colorado College professor who has a Ph.D. in microbiology from Harvard University.
Residents opposed to masks are also more likely to be opposed to getting vaccinated and that could create a problem, she said.
“We are going to see some people who are going to cheat the system,” she said.
In particular, communities with overall low vaccination rates could become hot spots and have trouble getting to a low level of viral spread, she said. The more the virus is transmitted the more likely it is to continue mutating into new variants, she said.
The state health department and the governor’s office did not respond to requests for comment.